UnitedHealthcare Choice Plus is in network for the New York City Employees PPO Plan
Update
Last modified: Feb. 27, 2026
Update: Additional information about network coverage area, payer ID numbers and resources
What to know about the NYCE PPO Plan
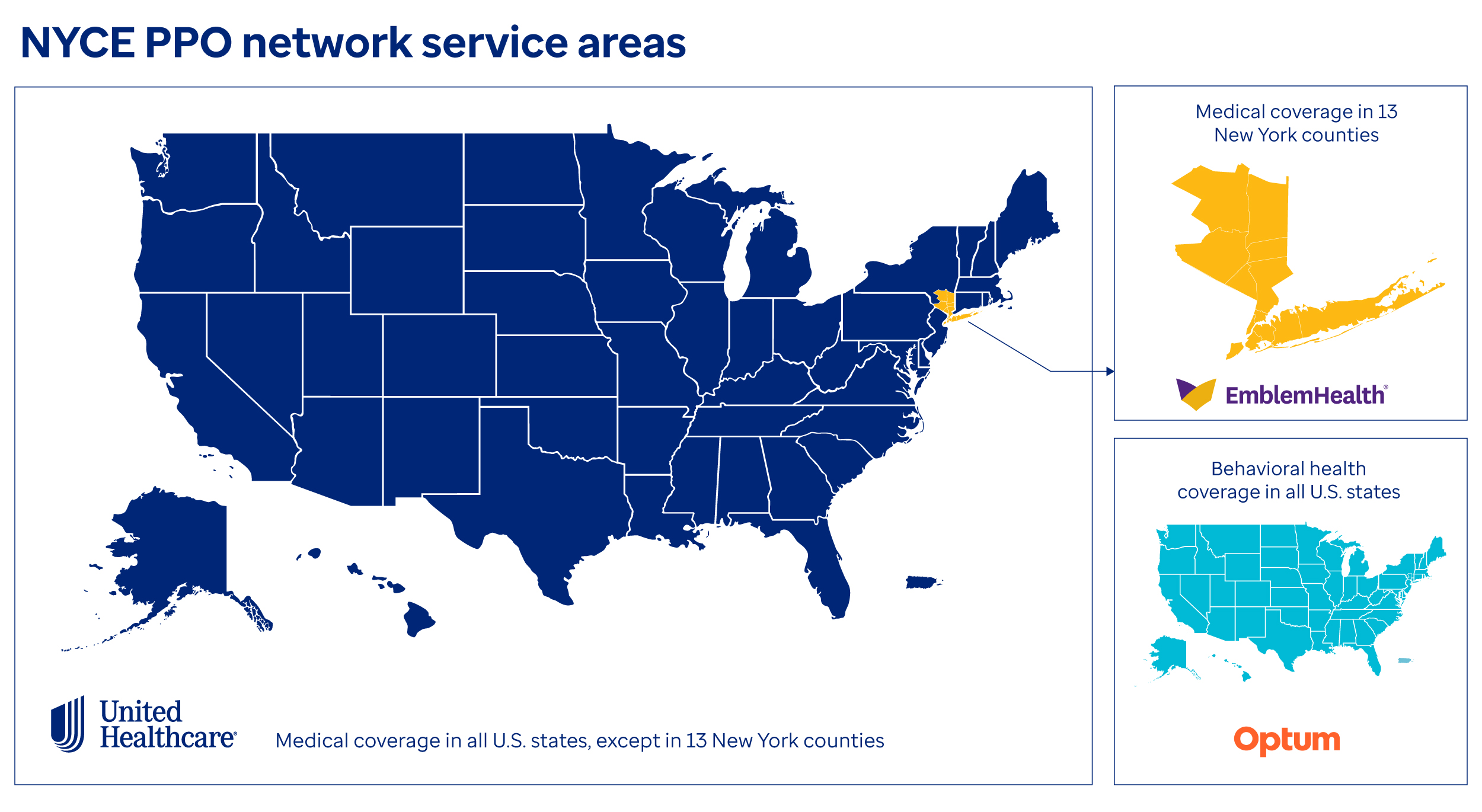
The New York City Employees PPO (NYCE PPO) plan, available in all U.S. states, offers provider network access through EmblemHealth Bridge Program, UnitedHealthcare Choice Plus and Optum Behavioral Health* to New York City employees, pre-Medicare retirees and their eligible dependents.
NYCE service areas and reimbursement rates
Providers are in network for NYCE PPO, as follows:
- EmblemHealth Bridge Program – Provider reimbursement rates apply for covered medical services rendered in the following 13 downstate New York counties:
– Bronx
– Duchess
– Kings
– Nassau
– New York
– Orange
– Putnam
– Queens
– Richmond
– Rockland
– Suffolk
– Ulster
– Westchester
- UnitedHealthcare Choice Plus – Provider reimbursement rates apply for covered medical services provided throughout the U.S., except in the 13 downstate New York counties covered by EmblemHealth Bridge
- Optum Behavioral Health – Provider reimbursement rates apply for covered behavioral health services provided throughout the U.S., including the downstate 13 New York counties listed above
Payer IDs for EDI claims and payments
EmblemHealth Bridge Program, UnitedHealthcare Choice Plus and United Behavioral Health use the same Electronic Data Interchange (EDI) payer ID codes. Ensure your EDI clearinghouse is set up for the following transactions:
- Submit EDI 837 claims using payer ID 26992
- Enable EDI 835 payments from payer ID 39026
NYCE PPO provider portal
Whether you’re contracted with EmblemHealth Bridge Program, UnitedHealthcare Choice Plus or United Behavioral Health, you must use the NYCE PPO provider portal to verify member eligibility, submit claims, request prior authorizations and other plan transactions. The UnitedHealthcare Provider Portal and the UMR Provider Portal do not provide access to the NYCE PPO Plan or member information.
Additional resources
Questions? We’re here to help.
Call NYCE PPO Provider Services at 844-849-5750 or chat with us through the NYCE PPO provider portal. If you need help setting up your clearinghouse transactions, contact the Payer ID Provider Support team at 866-678-8646, Monday–Friday, 8 a.m.–7 p.m. ET.
* United Behavioral Health operating under the brand Optum. In California, U.S. Behavioral Health Plan, California doing business as Optum and OptumHealth Behavioral Solutions of California.
PCA-1-26-00242-E&I-WEB_02192026